Interprofessional education program's goal is to reduce medical errors
March 13, 2019
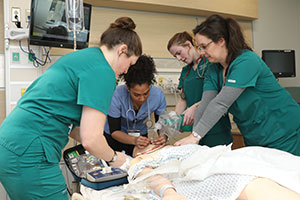
A respiratory student works with nursing students to stabilize a patient during an interprofessional education workshop at the Health Sciences Clinical Simulation Laboratory at the Flanagan Campus in Lincoln.
According to recent studies, medical errors are the third-leading cause of death in the United States, prompting an initiative to increase communication and collaboration among health care professionals.
The Community College of Rhode Island is joining the cause with the launch of its interprofessional education program, the first of its kind in the college’s 55-year history.
The program, known as IPE, brings together students from various fields in the school’s Health and Rehabilitative Sciences Department – from nurses and dental assistants to respiratory and emergency medical technicians – for a one-day workshop each semester to promote teamwork and help future health care professionals develop a better understanding of what others in the workforce do to streamline the patient care process. The project is funded by the state’s Executive Office of Health and Human Services Healthcare Workforce Transformation Initiatives grant.
“Studies show a decrease in errors when you have interprofessional education,” said Dr. Suzanne Carr, who was hired as the school’s IPE consultant and since has been named interim dean of Health and Rehabilitative Sciences.
“What’s amazing about CCRI,” added Kristen Fournier, the school’s program director for the Healthcare Workforce Transformation Initiative, “is that we have health care programs such as histotechnician, X-ray technician, opticianry, renal dialysis, etc., which provides an opportunity for all the schools to collaborate in ways that would not be possible individually. The educational aspects of working with these groups is endless. If we bring these groups together in an interprofessional sense, this would give the students in those programs an experience they haven’t had before.”
The larger goal is to make IPE sustainable at CCRI, which is why the school brought in Carr, an IPE “guru,” said Fournier. Carr completed her doctorate research on IPE and also developed IPE curriculum at the New England Institute of Technology.
“It’s not just one person or one department. It’s the buy-in to make sure that people are also realizing the importance of it,” Carr said. “We all know it needs to be done. The faculty as a whole knows the importance of working together with the disciplines.”
IPE does not add additional courses to the students’ existing curriculum. Instead, these one-day workshops are woven into the current course load. CCRI implemented its IPE trial run in the fall with a workshop for nursing and respiratory students – more than 100 total divided into groups of eight – and continued this month with another collaborative designed for dental, EMT and nursing students in which a dental patient experienced shortness of breath or dizziness during a routine procedure.
In the simulation, the dental students had to decide how to stabilize the patient and then, upon calling 911, properly communicate what was happening to the EMT students. The patient was brought to the emergency room, where communication again becomes key as the EMT students worked hand in hand with nursing students to properly stabilize the patient.
“That’s what we’re capitalizing on – that interaction,” Carr said. “They’re finding that when they’re in these situations, ‘Could you have delegated that skill? Could you have improved communication because you realized the task wasn’t done?’”
Students participate in a separate case study with a team-building exercise in which the students work with dry strands of spaghetti and marshmallows using basic engineering principles to build the tallest structure. Students also complete voluntary pre- and post-lab surveys, allowing faculty to gauge the effectiveness of the curriculum and determine the students’ understanding of the four core competencies of IPE – value and ethics, role and responsibility, interprofessional communication, and teamwork and collaboration – all of which are important in reducing medical errors in the workforce.
A recent Johns Hopkins study said more than 250,000 Americans die each year from medical errors. Similar studies show a correlation between nurse-to-patient ratios and employee satisfaction and patient care. More than 75 percent of registered nurses participating in a 2018 survey commissioned by the Massachusetts Nurses Association believed nurses were assigned too many patients at one time. Sixty-four percent of the RNs in that same survey reported an increase in patient injury due to understaffing and 77 percent reported medication errors due to unsafe patient assignments.
Likewise, the global management firm McKinsey & Co. recently conducted a case study at a military hospital and determined that improved work conditions resulted in reduced absentee rates among nurses and a significant decrease in medical errors.
“Without IPE, students are at a disadvantage when entering the health care workforce,” Fournier said. “They learn their particular discipline, they take their licensure exams and they work in their respective fields. They’re expected to work closely with other health care professionals and understand what they do. Having this early exposure, this connection with their peers, and being able to recognize and respect the roles and competencies of everyone they’re working with makes a safer and more productive workforce.”
The IPE initiative eventually may expand, giving students the potential for two IPE experiences before they graduate. The next step is working on new simulations and case studies to include all – or most – of the HARS programs for future workshops, whether it’s physical therapy, occupational therapy or opticianry. There is also the potential to include the school’s Human Services Department and work with students majoring in social services or early childhood development.
“The overall goal is to work together. Collaboration is a very big term that we use,” Carr said. “We know we can work together. We want to try to improve role recognition, communication skills and teamwork. That’s all part of the plan. We’re not necessarily teaching them something new. We’re just playing on their previous knowledge and hoping to enhance it.”